Lower Limb Wounds
What Are Lower Limb Wounds?
Lower limb wounds are injuries or chronic ulcers that develop on the legs, ankles, or feet and fail to heal within a normal timeframe. These wounds often occur when circulation is reduced, tissue health is compromised, or underlying medical conditions interfere with the body’s natural repair process.
The lower extremities carry body weight and endure daily pressure, movement, and friction. Because of this constant stress, even minor skin injuries such as a small cut, blister, or abrasion can worsen quickly if blood flow is inadequate or healing capacity is reduced. When recovery is delayed, the wound may enlarge, deepen, or become infected.
If not properly treated, lower limb wounds can progress into chronic ulcers that persist for months or longer. These wounds are particularly concerning because they can serve as entry points for bacteria, increasing the risk of cellulitis, abscess formation, bone infection, and other systemic complications.
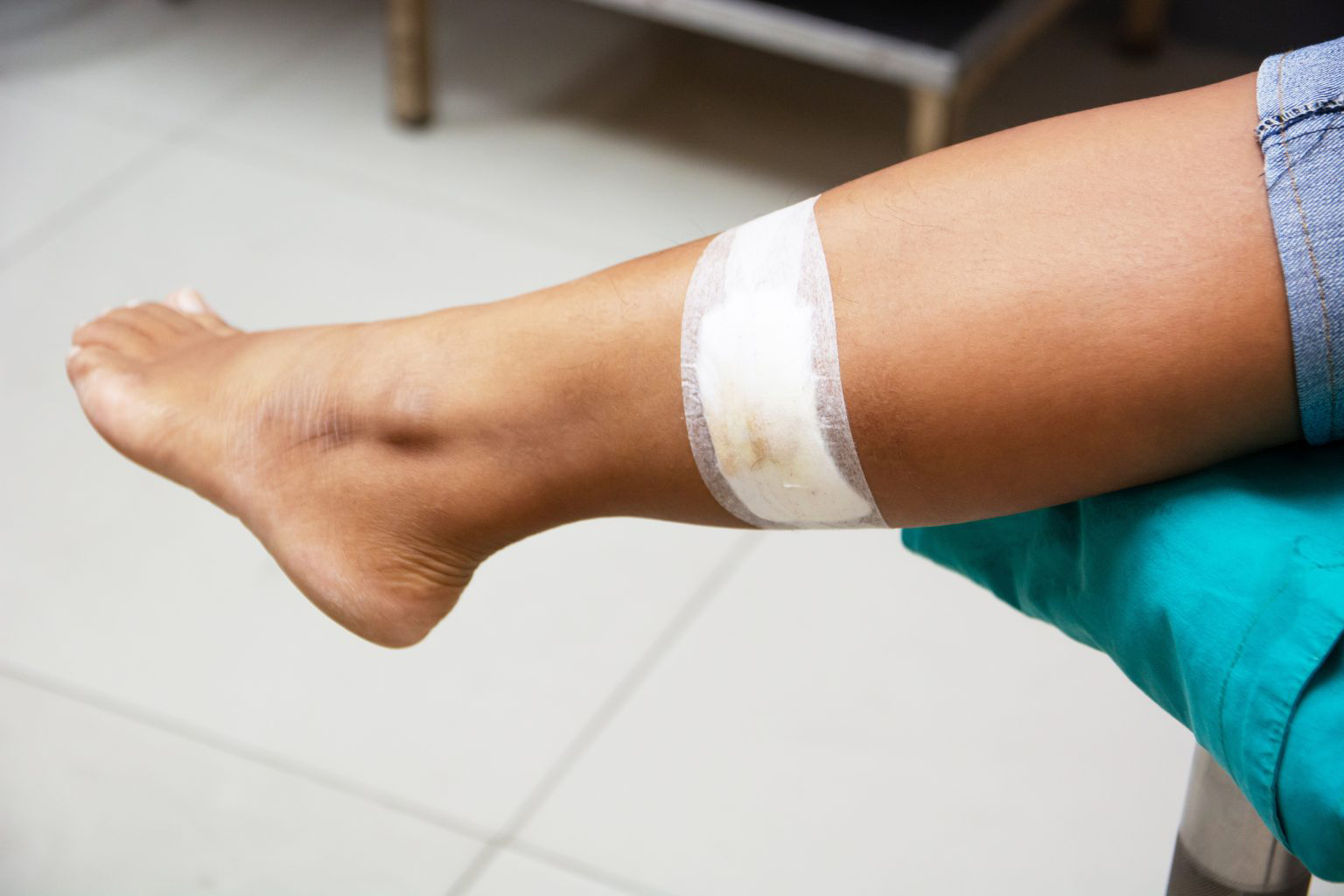
What Are the Causes
Lower limb wounds usually develop due to a combination of circulatory problems, chronic disease, mechanical stress, and tissue vulnerability.
Venous insufficiency is one of the most common causes. When leg veins cannot efficiently return blood to the heart, pressure builds within the lower limbs. This leads to swelling, skin discoloration, and fragile tissue that is more prone to breakdown and ulcer formation.
Diabetes is another significant contributor. Elevated blood glucose levels over time damage blood vessels and nerves, impair immune response, and reduce the body’s ability to heal. As a result, small unnoticed injuries may evolve into chronic wounds.
Arterial disease, which restricts oxygen rich blood from reaching tissues, also plays a major role. Trauma from falls, sharp objects, repetitive friction, or prolonged pressure can initiate wounds, especially in individuals with poor circulation or reduced mobility.
Autoimmune disorders such as rheumatoid arthritis or vasculitis may weaken blood vessels or trigger inflammation that damages skin integrity. Additional risk factors include obesity, smoking, advanced age, prolonged standing, and infection. In most cases, wounds develop when several of these factors occur together.
Symptoms
Lower limb wounds may begin as small superficial injuries but can progress into deeper ulcers when healing is impaired. Early signs often include redness, swelling, warmth, or skin discoloration. The area may appear irritated or fragile before the skin fully breaks down.
As the wound progresses, individuals may notice drainage, crusting, thickened edges, or visible underlying tissue. Some wounds appear shallow with irregular borders, particularly those related to venous disease. Arterial ulcers are often deeper and may have a pale or darkened base due to reduced blood supply.
Pain is common, although individuals with neuropathy may experience minimal discomfort despite significant tissue damage. Signs of infection include foul odor, increased drainage, spreading redness, fever, or fatigue.
Changes in the surrounding skin, such as tightness, shininess, or inflammation, may indicate worsening circulation. Early recognition and medical evaluation are essential to prevent serious complications.
How Many People Are Affected?
Lower limb wounds represent a substantial public health concern worldwide. In the United States alone, more than 8 million people are estimated to live with chronic wounds, and a significant portion involve the lower extremities.
Venous leg ulcers affect approximately 1 to 3 percent of the population, while diabetic and arterial related lower limb wounds impact millions globally. According to the World Health Organization, the global rise in diabetes and vascular disease has contributed to increasing rates of chronic lower extremity wounds.
Adults over the age of 65 are particularly vulnerable due to reduced mobility, impaired circulation, and multiple coexisting medical conditions. Recurrence rates are high, especially for venous and diabetic ulcers, highlighting the need for long term management and preventive care.
Complications
If left untreated, lower limb wounds can lead to significant complications. Infection is one of the most immediate concerns. Bacteria can spread into deeper tissues, potentially resulting in cellulitis, abscess formation, or bone infection.
Chronic wounds may progressively enlarge and destroy surrounding healthy tissue. Reduced mobility, persistent pain, and loss of independence are common consequences. In severe cases, particularly when circulation is severely compromised, tissue death may occur and surgical intervention may be required.
Recurrent ulcers are common when underlying conditions such as venous insufficiency, arterial disease, or diabetes are not effectively managed. Emotional stress and reduced quality of life often accompany prolonged wound healing.
Early diagnosis and comprehensive care are critical to preventing long term damage and preserving mobility.
Diagnosis
Assessment of a lower limb wound involves a detailed clinical evaluation. Healthcare providers examine the size, depth, appearance, and location of the wound while assessing for signs of infection.
Vascular testing may be performed to evaluate blood flow and determine whether venous or arterial disease is present. Blood tests may help assess glucose control, inflammation, or infection. Imaging studies can be recommended if deeper tissue or bone involvement is suspected.
Identifying the underlying cause is essential to guide appropriate treatment and improve healing outcomes.
Treatment Options
Management of lower limb wounds focuses on improving circulation, supporting tissue repair, controlling infection, and reducing mechanical stress.
Standard wound care includes gentle cleansing, removal of non viable tissue when necessary, and application of appropriate dressings to maintain a balanced healing environment. Offloading pressure from the affected area is critical, especially for wounds on the foot or ankle.
Compression therapy may be used for venous ulcers to improve blood return, while revascularization procedures may be necessary in cases of arterial insufficiency. Blood sugar control is essential in individuals with diabetes.
In advanced wound care settings, regenerative therapies such as Stem Cells and Exosomes are being explored to enhance healing at the cellular level. These therapies aim to stimulate new blood vessel formation, reduce inflammation, encourage collagen production, and promote tissue regeneration in chronic or non healing wounds.
Nutritional support, smoking cessation, mobility improvement, and regular follow up are important for long term success. A multidisciplinary approach often provides the best outcomes for complex lower limb wounds.
Trusted Resources
SCHEDULE A CONSULTATION
Request a Physician Evaluation
Submit your information to connect with a participating physician in your region to determine whether regenerative therapy may be appropriate for your condition.

