Diabetic Foot Ulcers (DFUs)
What Are Diabetic Foot Ulcers?
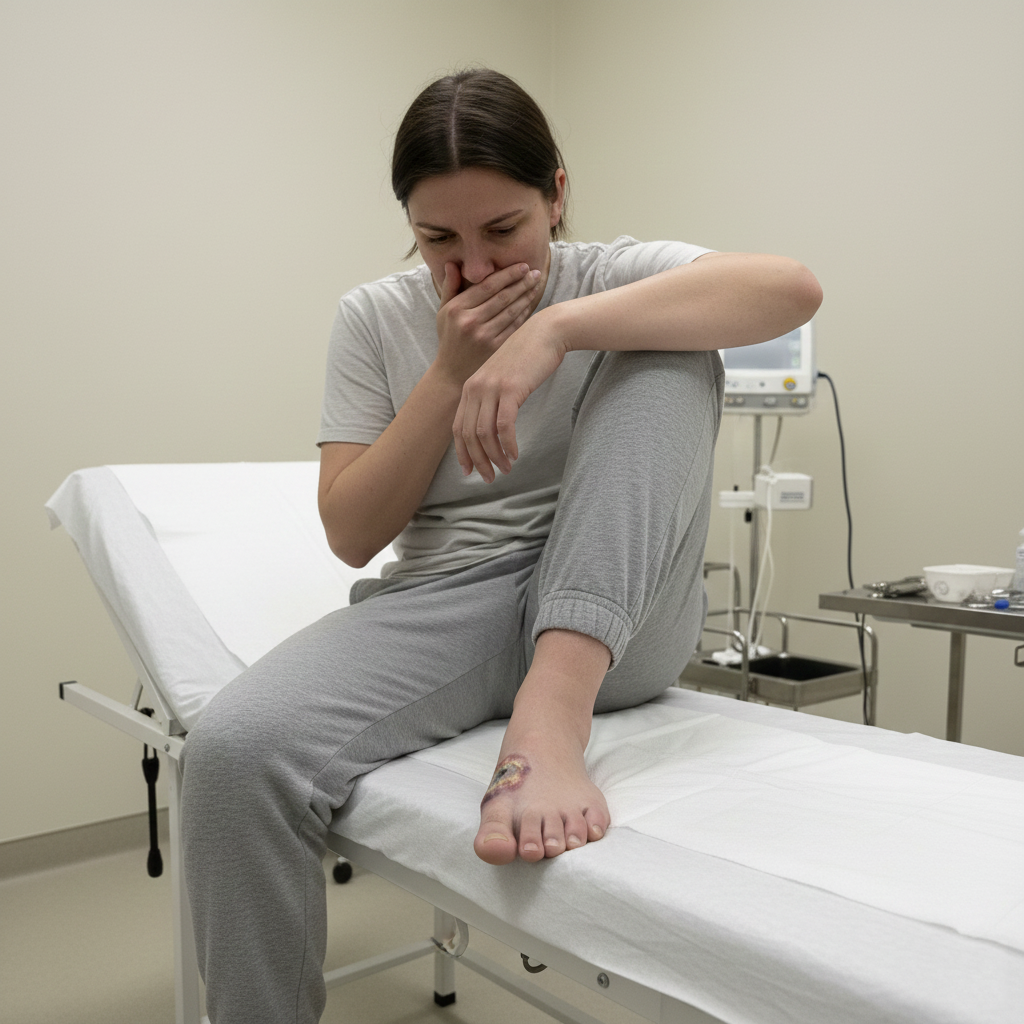
Diabetic Foot Ulcers are chronic, non healing wounds that develop on the feet of individuals living with diabetes. They occur when elevated blood sugar levels over time damage nerves and blood vessels, reducing sensation and impairing circulation. As a result, even small injuries such as a blister, cut, or pressure spot may fail to heal properly and gradually progress into an open sore.
These ulcers commonly appear on weight bearing areas of the foot, including the heel, toes, and the ball of the foot. Because diabetic neuropathy reduces the ability to feel pain, many people do not notice the injury until it becomes more advanced. Over time, the wound may extend deeper into tissue layers and, in severe cases, expose muscle or bone.
Diabetic foot ulcers are considered one of the most serious complications of diabetes because they are slow to heal and highly vulnerable to infection. Early understanding and proactive foot care are essential to protect mobility and overall quality of life.
What Are the Causes
Diabetic foot ulcers develop due to a combination of nerve damage, poor circulation, and weakened immune function associated with diabetes.
Peripheral neuropathy reduces sensation in the feet, making it difficult to detect minor trauma, pressure, or irritation. Without protective pain signals, repeated stress on the skin may cause breakdown and ulcer formation.
Reduced blood flow is another major factor. Diabetes can cause narrowing and hardening of blood vessels, limiting oxygen and nutrient delivery to tissues. When circulation is compromised, the body cannot repair damaged skin efficiently, resulting in delayed healing.
Elevated blood glucose levels also weaken the immune system, increasing susceptibility to infection once a wound forms. Mechanical factors such as ill fitting footwear, foot deformities, limited joint mobility, callus buildup, or abnormal walking patterns further increase risk.
Preventing diabetic foot ulcers involves routine foot inspection, proper footwear, good hygiene, and consistent blood sugar management.
Symptoms
Diabetic foot ulcers often begin gradually. Early signs may include redness, warmth, swelling, or a localized area of pressure on the foot. The skin may eventually break down, forming an open sore surrounded by inflammation.
The ulcer may appear shallow at first but can deepen over time. Drainage or fluid discharge is common. The wound tissue may look pale, yellowish, or darkened depending on circulation and infection status. A foul odor can indicate bacterial involvement.
Some individuals notice thickened skin or callus formation before an ulcer develops. If infection spreads, symptoms such as fever, chills, or fatigue may occur. Even in the absence of pain, any persistent wound in a person with diabetes requires prompt medical evaluation.
How Many People Are Affected?
Diabetic foot ulcers represent a significant global health issue. Research suggests that approximately 15 to 25 percent of individuals with diabetes will develop a foot ulcer during their lifetime. Each year, millions of new cases are reported worldwide.
According to the World Health Organization, the rising global prevalence of diabetes has contributed to an increase in related complications, including foot ulcers. These wounds are among the leading causes of diabetes related hospital admissions and account for a large proportion of non traumatic lower limb amputations.
Both type 1 and type 2 diabetes carry risk, particularly in individuals with long standing disease, poor glucose control, cardiovascular complications, or established neuropathy. Older adults and those with limited mobility are especially vulnerable.
Complications
If not treated appropriately, diabetic foot ulcers can lead to serious complications. Infection is one of the most immediate concerns. Due to impaired immune function, bacteria can spread quickly into surrounding tissues.
Untreated infections may progress to cellulitis, abscess formation, bone infection, or systemic illness. In cases of severe circulation impairment, tissue death may occur, increasing the risk of gangrene.
Chronic ulcers can significantly reduce mobility, limit independence, and affect emotional well being. Recurrent ulcers are common when underlying neuropathy or vascular disease remains unmanaged.
In advanced cases, partial or complete amputation of the affected limb may become necessary. Although many amputations are preventable with early intervention and proper wound management, they remain a major complication worldwide.
Diagnosis
Diagnosing a diabetic foot ulcer begins with a thorough clinical assessment. Healthcare providers evaluate the size, depth, location, and appearance of the wound, as well as signs of infection or tissue damage.
A neurological examination may assess sensation loss, while vascular testing evaluates blood flow to the foot. Blood tests can help determine glucose control and identify signs of infection. Imaging studies may be recommended if bone involvement or deeper structural damage is suspected.
Accurate diagnosis allows for targeted treatment planning and reduces the risk of complications.
Treatment Options
Management of diabetic foot ulcers focuses on promoting wound healing, preventing infection, and addressing the underlying causes that interfere with recovery.
Wound care typically includes careful cleaning, removal of non viable tissue, and application of appropriate dressings to maintain a supportive healing environment. Offloading pressure from the affected area is critical. This may involve specialized footwear, orthotics, padding, or casting techniques designed to redistribute weight away from the ulcer.
Strict blood sugar control plays a central role in improving healing outcomes. When infection is present, antibiotics may be required based on clinical evaluation.
In advanced wound care settings, regenerative therapies such as Stem Cells and Exosomes are being explored to support tissue repair at a cellular level. These therapies aim to enhance blood vessel formation, reduce inflammation, and stimulate the regeneration of damaged tissue, particularly in wounds that have not responded to conventional treatment.
Improving circulation, optimizing nutrition, smoking cessation, and routine follow up are essential components of comprehensive care. Ongoing education and preventive foot monitoring help reduce recurrence.
Trusted Resources
SCHEDULE A CONSULTATION
Request a Physician Evaluation
Submit your information to connect with a participating physician in your region to determine whether regenerative therapy may be appropriate for your condition.

