Burn Injury
What Is a Burn Injury?
A burn injury is a type of tissue damage that occurs when the skin or underlying structures are exposed to heat, chemicals, electricity, radiation, or friction. Burns can range from mild surface injuries affecting only the outer layer of skin to deep wounds that extend into muscle, tendons, or bone.
The skin serves as the body’s primary protective barrier. It regulates temperature, prevents infection, and preserves essential fluids. When a burn disrupts this barrier, the impact goes beyond the visible wound. The body initiates a complex healing response that may involve inflammation, fluid shifts, immune activation, and systemic stress.
Burns are categorized according to depth. First degree burns involve only the outer layer of skin and typically cause redness and discomfort. Second degree burns extend deeper, often producing blisters and significant pain. Third degree burns destroy the full thickness of the skin and may appear pale, leathery, or charred, sometimes with reduced sensation due to nerve damage. In severe cases, fourth degree burns penetrate into muscle or bone and require urgent medical intervention.
Because burn injuries affect both physical and emotional well being, comprehensive care is essential for restoring function and improving long term recovery.
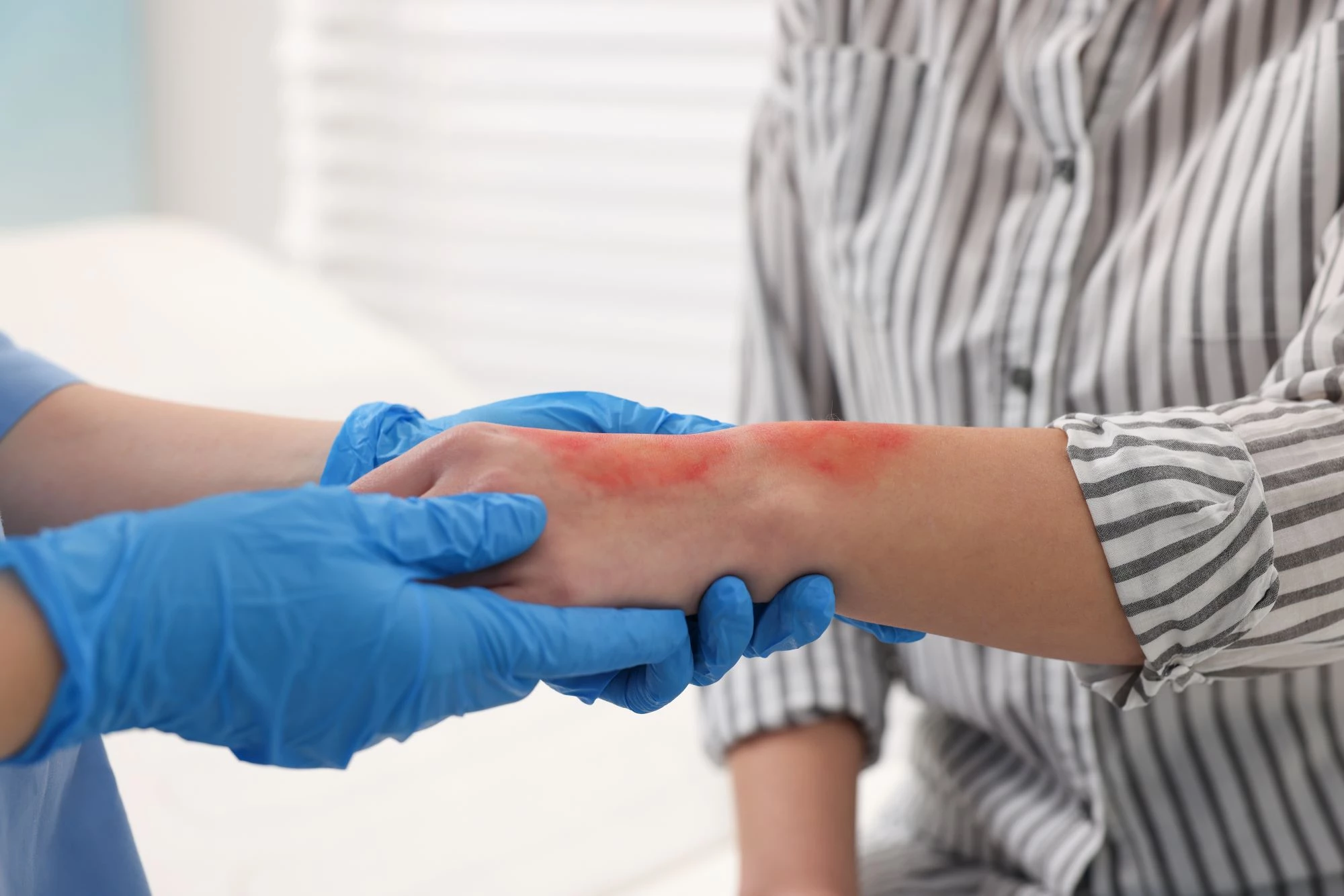
What Are the Causes
Burn injuries result from several different external sources, each producing distinct patterns of tissue damage.
Thermal burns are the most common and occur from contact with flames, hot liquids, steam, or heated surfaces. Scald injuries frequently affect children and older adults. Flame burns are often associated with residential fires, cooking accidents, or workplace incidents.
Chemical burns develop after exposure to corrosive substances such as acids, alkalis, cleaning agents, or industrial compounds. These injuries may continue to damage tissue until the chemical is fully removed.
Electrical burns occur when an electrical current passes through the body. Although the external wound may appear small, internal tissue damage can be extensive. Radiation burns may arise from prolonged sun exposure, medical treatments, or industrial radiation sources. Friction burns result from forceful contact with rough surfaces, such as pavement or machinery.
Underlying health conditions can influence severity and healing outcomes. Poor circulation, diabetes, immune dysfunction, advanced age, and chronic illness may slow recovery and increase complication risk.
Symptoms
The signs of a burn injury vary depending on depth and severity. Mild burns often present with redness, tenderness, and localized swelling. Deeper burns may cause blistering, fluid leakage, intense pain, or changes in skin texture.
Second degree burns typically appear moist and bright red with blister formation. Third degree burns may look white, brown, or charred and can feel numb due to nerve destruction. In extreme cases, muscle or bone may be visible.
As the injury progresses, swelling, stiffness, and restricted movement may occur. Burns involving the face, neck, chest, hands, or joints can significantly interfere with breathing or mobility. Burns that encircle a limb or torso may restrict circulation or chest expansion.
Systemic symptoms such as fever, chills, nausea, or fatigue may indicate infection or a broader inflammatory response. Emotional reactions including anxiety, distress, and psychological trauma are also common and should not be overlooked.
How Many People Are Affected?
Burn injuries remain a significant global health concern. According to the World Health Organization, millions of people require medical care for burns each year, with approximately 180,000 deaths occurring annually worldwide. Many of these fatalities occur in regions where access to specialized burn care is limited.
In the United States alone, hundreds of thousands of burn injuries require medical treatment each year, and tens of thousands result in hospitalization. Children, older adults, and individuals with limited mobility are at increased risk.
The financial and social impact of burn injuries is substantial, often requiring extended hospitalization, surgical procedures, rehabilitation, and long term scar management.
Complications
Burn injuries can lead to serious short and long term complications. Infection is one of the most immediate risks because damaged skin no longer provides adequate protection against bacteria. Severe infections may progress to systemic illness if not treated promptly.
Deep burns can cause significant tissue loss and may require skin grafting or reconstructive surgery. Excessive scar formation is common. Hypertrophic scars and keloids may develop due to abnormal collagen production during healing. Contractures, where tightening of scar tissue restricts joint movement, can limit flexibility and physical function.
Burns affecting the airway may cause respiratory complications, especially in cases involving smoke inhalation. Circulatory disturbances and blood clot risk may also increase in severe injuries.
Psychological challenges, including depression, anxiety, and post traumatic stress, are frequently reported among burn survivors. Long term rehabilitation often addresses both physical and emotional recovery.
Diagnosis
Evaluation of a burn injury begins with assessing the depth, size, and location of the wound. Healthcare providers determine the percentage of body surface area involved and classify the burn according to severity.
Additional evaluation may include monitoring vital signs, fluid balance, and signs of infection. Laboratory testing may be used in moderate to severe burns to assess electrolyte levels, organ function, and systemic response. Imaging studies may be recommended when deeper structural involvement is suspected.
Early and accurate assessment guides treatment decisions and improves outcomes.
Treatment Options
Treatment of burn injuries focuses on protecting the wound, preventing infection, supporting tissue repair, and minimizing scarring.
Initial management includes gentle cleansing, removal of non viable tissue when necessary, and application of appropriate dressings to maintain a supportive healing environment. Fluid management and pain control are critical in moderate to severe burns.
In advanced wound care settings, regenerative therapies such as Stem Cells and Exosomes are being explored to enhance healing at a cellular level. Stem cells may support tissue regeneration by promoting new blood vessel formation, reducing inflammation, and stimulating repair of damaged skin structures. Exosomes contribute to cellular communication and may enhance collagen production, angiogenesis, and overall wound recovery.
Rehabilitation, scar management, nutritional optimization, and psychological support are essential components of comprehensive burn care. Long term follow up helps maintain mobility, improve cosmetic outcomes, and reduce the risk of complications.
Trusted Resources
SCHEDULE A CONSULTATION
Request a Physician Evaluation
Submit your information to connect with a participating physician in your region to determine whether regenerative therapy may be appropriate for your condition.

