Chronic Low Back Pain
What Is Chronic Low Back Pain?
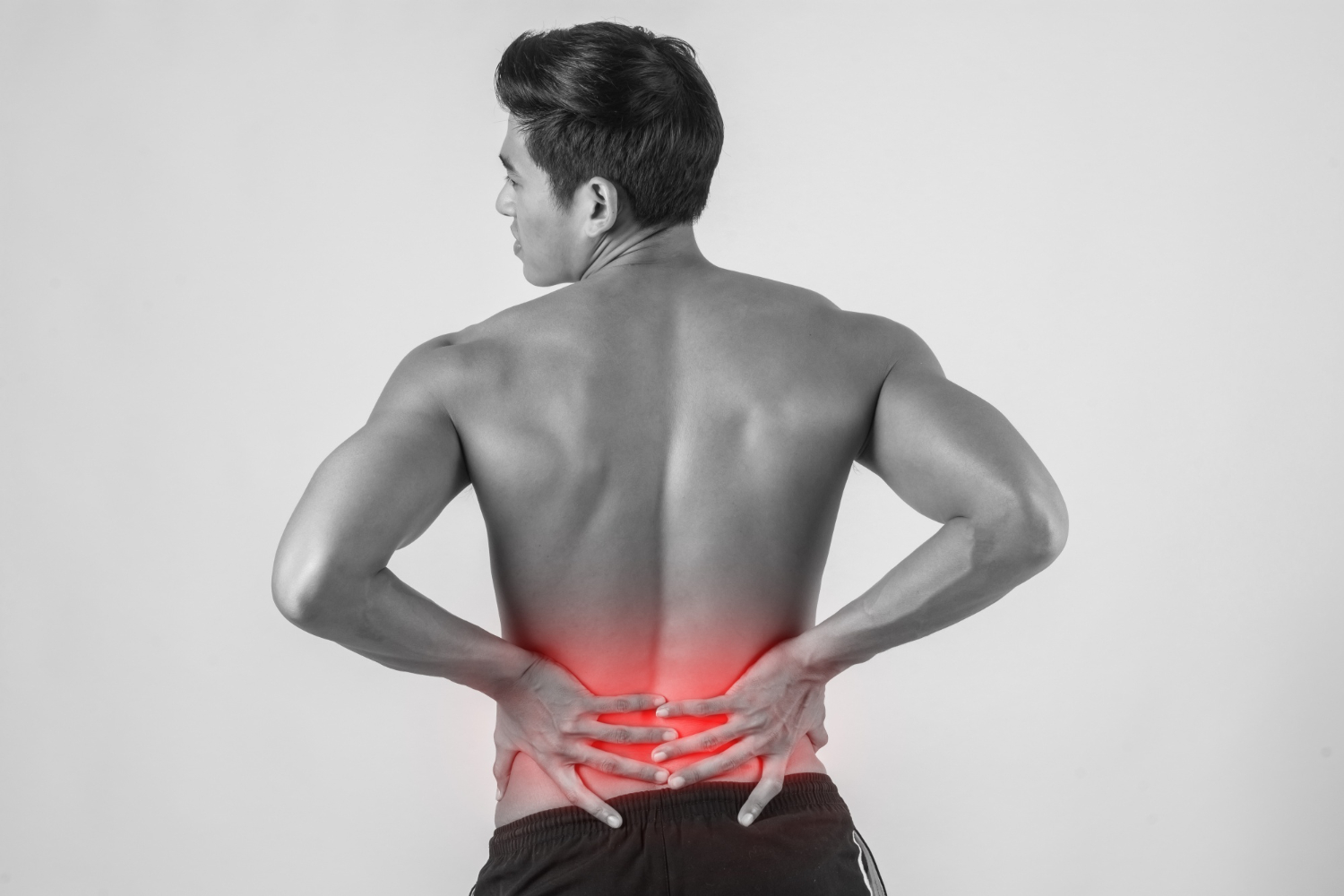
Chronic low back pain refers to persistent discomfort in the lumbar spine lasting longer than three months. Unlike acute back pain, which often resolves with short-term rest and conservative care, chronic low back pain may involve ongoing structural degeneration, mechanical instability, or sustained inflammation affecting spinal tissues.
The lower back supports body weight, facilitates movement, and protects critical nerve structures. Because it absorbs significant mechanical stress during bending, lifting, twisting, and prolonged sitting, it is particularly vulnerable to cumulative strain over time.
Chronic low back pain may originate from intervertebral discs, facet joints, ligaments, paraspinal muscles, or nerve roots. In many individuals, multiple structures contribute simultaneously, creating a complex and persistent pain pattern.
What Are the Causes
Symptoms vary depending on the underlying structures involved. Pain is often described as aching, stiffness, or deep soreness localized in the lower back. Some individuals experience intermittent flare-ups triggered by prolonged sitting, bending, or lifting.
When nerve involvement is present, pain may radiate into the buttocks or legs. Stiffness is common in the morning or after inactivity. Reduced flexibility and difficulty with prolonged standing or walking may develop over time.
Muscle guarding may occur as the body attempts to protect the affected area, further limiting mobility. Chronic cases may involve persistent low-grade discomfort punctuated by more intense episodes.
Symptoms
Symptoms vary depending on the underlying cause.
Individuals may experience deep groin discomfort during walking, pivoting, or prolonged sitting. Lateral hip pain may worsen when lying on the affected side. Mechanical symptoms such as clicking, catching, or locking can suggest labral involvement.
Stiffness and limited range of motion may develop gradually. Activities such as climbing stairs, rising from a seated position, or bending may become uncomfortable. In degenerative cases, pain may persist at rest or during nighttime.
When inflammation is present, swelling and localized tenderness may occur. Chronic cases can lead to compensatory movement patterns affecting the lower back or opposite hip.
How Many People Are Affected?
Chronic low back pain is one of the leading causes of disability worldwide.
It is estimated that up to 80 percent of adults experience low back pain at some point in their lives, and a significant percentage develop chronic symptoms lasting longer than three months. Adults between ages 30 and 65 are most frequently affected.
Sedentary lifestyles, aging populations, and occupational strain contribute to the high prevalence of chronic lumbar pain globally.
Complications
If left untreated, chronic low back pain may lead to progressive functional limitation. Persistent inflammation and mechanical instability can accelerate disc degeneration and facet joint arthropathy.
Reduced activity due to pain may result in muscle deconditioning, further destabilizing the spine. Compensation patterns may place additional stress on the hips, pelvis, and thoracic spine.
Chronic pain may also affect sleep quality, physical activity levels, and overall quality of life. In advanced cases, structural deterioration may increase the risk of recurrent nerve compression.
Early evaluation and targeted management reduce the risk of progressive spinal dysfunction.
Diagnosis
Diagnosis begins with a comprehensive history and physical examination. A healthcare provider evaluates posture, spinal mobility, muscle strength, neurologic function, and pain patterns.
Imaging studies may be used to identify structural contributors. X-rays assess spinal alignment and degenerative changes. MRI provides detailed visualization of discs, nerve roots, and facet joints.
At Victory Over Pain, Diagnostic Ultrasound may assist in evaluating superficial paraspinal soft tissue involvement and guide image-directed regenerative procedures when appropriate.
Accurate diagnosis integrates clinical findings with imaging to determine the primary pain generators and guide individualized treatment planning.
Treatment Options
Treatment focuses on improving spinal stability, reducing inflammation, and restoring functional mobility.
Structured physical therapy emphasizing core stabilization, posture correction, and controlled spinal loading remains foundational. Activity modification and ergonomic adjustments help reduce repetitive mechanical strain.
Low-Level Light Therapy (LLLT) may be incorporated as a non-invasive modality to support cellular energy production and modulate inflammatory signaling in soft tissue–related lumbar pain patterns.
Extracorporeal Shockwave Therapy (ESWT) may be considered in select cases where chronic muscular or ligamentous degeneration contributes to persistent pain.
When disc-related or facet-mediated inflammation persists, Platelet-Rich Plasma (PRP) therapy may be evaluated to support biologic modulation under image guidance.
In selected individuals with advanced degenerative disc pathology or chronic structural instability, MSC-derived exosome therapy or stem cell therapy may be evaluated to support regenerative signaling within affected spinal segments.
Surgical intervention is typically reserved for cases involving progressive neurologic deficits, structural instability, or failure of comprehensive conservative and regenerative strategies.
Modern spine care emphasizes early intervention, individualized treatment planning, and preservation of long-term spinal integrity.
Trusted Resources
SCHEDULE A CONSULTATION
Request a Physician Evaluation
Submit your information to connect with a participating physician in your region to determine whether regenerative therapy may be appropriate for your condition.

